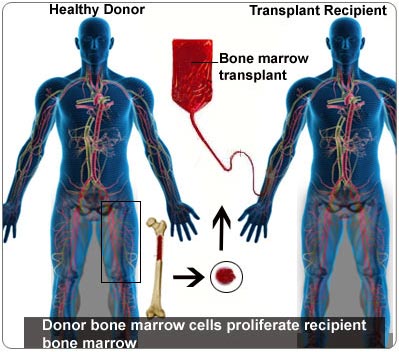
Bone Marrow Transplant
A bone marrow transplant is a procedure to replace damaged or destroyed bone marrow with healthy bone marrow stem cells. Bone marrow is the soft, fatty tissue inside your bones. Stem cells are immature cells in the bone marrow that give rise to all of your blood cells.
Hematopoietic stem cell transplantation (HSCT) is the transplantation of multipotent hematopoietic stem cell or blood, usually derived from bone marrow, peripheral blood stem cells, or umbilical cord blood. Stem cell transplantation is a medical procedure in the fields of hematology and oncology, most often performed for people with diseases of the blood, bone marrow, or certain cancers.
Hematopoietic stem cell transplantation remains a risky procedure with many possible complications; it has traditionally been reserved for patients with life-threatening diseases. While occasionally used experimentally in nonmalignant and nonhematologic indications such as severe disabling auto-immune disease and cardiovascular disease, the risk of fatal complications appears too high to gain wider acceptance.
In patients with leukemia, aplastic anemia, and some immune deficiency diseases, the stem cells in the bone marrow malfunction, producing an excessive number of defective or immature blood cells (in the case of leukemia) or low blood cell counts (in the case of aplastic anemia). The immature or defective blood cells interfere with the production of normal blood cells, accumulate in the bloodstream and may invade other tissues.
Large doses of chemotherapy and/or radiation are required to destroy the abnormal stem cells and abnormal blood cells. These therapies, however, not only kill the abnormal cells but can destroy normal cells found in the bone marrow as well. Similarly, aggressive chemotherapy used to treat some lymphomas and other cancers can destroy healthy bone marrow. A bone marrow transplant enables physicians to treat these diseases with aggressive chemotherapy and/or radiation by allowing replacement of the diseased or damaged bone marrow after the chemotherapy/radiation treatment.
There are three kinds of bone marrow transplants:
Autologous bone marrow transplant: "Auto" means "self." Immature marrow cells (stem cells) are removed from the patient himself before he receives high-dose chemotherapy or radiation treatment. After these treatments are done, the stems cells are put back in the body. This is called a "rescue" transplant.
Allogeneic bone marrow transplant: In this procedure stem cells are taken either by bone marrow harvest or apheresis from a genetically-matched donor, generally a brother or sister or parent. It can also be a unrelated bone marrow transplant when the donor is not a relative of the patient but his cells are matching genetically with the patient.
Umbilical cord blood transplant: In this type of transplant stem cells are taken from an umbilical cord immediately after delivery of an infant. These stem cells are than tested, typed, counted, and frozen until they are ready to be transplanted.
These are four stages involved in BMT.
Stage 1: Evaluate the patients for BMT (WORK-UP) usually 14-30 days before
One will undergo complete medical check-up to evaluate one’s suitability to go through the BMT procedure. This involves the following:
• Blood Tests
• Chest X- ray and CT Scans
• Tests to assess the condition of heart and lungs
• Bone Marrow Tests
Patients will be counselled in detail about the procedure, the complications, the chances of success, the cost and the possible length of stay in the hospital. Patient will be encouraged to go through the educational material/booklet and discuss any queries or doubts that he / She might have.
Stage2: Prepare the patient for BMT (CONDITIONING) usually 2-10 days
High dose of chemotherapy or radiotherapy is given to destroy the diseased marrow or destroy the cancer elsewhere and the bone marrow gets damaged as a result. This is needed to create space for new blood stem cell and also to suppress the patient’s own immune system (in case of allogeneic transplant), so that the blood stem cells are not rejected.
A Cadaveric Transplant the donor may be a victim of an accident or head injury. The donor's heart is still beating, but the brain has stopped functioning. Such a person is considered legally dead, because his or her brain has permanently and irreversibly stopped working. At this point, the donor is usually in an intensive-care unit.
The actual process of transplantation
The transplant procedure is actually fairly simple, the stem cells or bone marrow cells to be transplanted are given through the Central Venous line (CVL). The procedure is just like getting a blood transfusion, except the following precautions which has to be taken care of :
• Just before the infusion of the new bone marrow, the patient may be given medication to help avoid any allergic reactions.
• A monitor is used to check breathing, heart rate and blood pressure during the procedure. The nurse monitors closely throughout the infusion of stem cells or bone marrow.
• A doctor is available in the unit and will check the patient periodically. Medications may be given to deal with problems that may arise, such as high blood pressure or a fast heart rate.
Stage 3: Pre-engraftment (before the transplanted blood stem cells start working): (Usually 2-3 weeks)
After high dose chemo-radiotherapy the blood stem cells are destroyed and normal blood cells are not produced. The patients need to be kept in a clean room within the BMT unit in strict isolation during this time. They also need a lot of blood and platelet transfusion. Most patients get serious infections during this period and need treatment with antibiotics.
Stage 4: Post-engraftment (after the transplanted blood stem cells start working)
Early phase (first 3 months)
There are two types of white blood cells: neutrophils and lymphocytes. Neutrophils save us from acute infections and lymphocytes prevent repeated or chronic infections. Once the neutrophil count is above the critical value of 500 cells per microlitre, the patient can come out of critical isolation. This is called engraftment or the first sign that the transplanted blood stem cells are functioning. Soon after the neutrophil increase to normal or near-normal levels and if there is no other complication, the patient can be discharged home. However, regular check-up and blood tests (2-3 times a week) are required. There is also a risk of graft-versus-host disease (GVHD) at this stage.
Late Phase (3 months-12 months)
The immunity against viruses takes a very long time to recover. Even though some of the immunity is restored, the patient is still at risk of infections with viruses and fungus. This is more so if they are being treated for GVHD, which can become chronic and lingering. If the patient is well, the frequency of check-ups and blood tests reduce over several months.
A bone marrow transplant is usually done in a hospital or medical center that specializes in such treatment. Most of the time, you will stay in a special bone marrow transplant unit in the center to limit your chance of getting an infection. All or part of an autologous or allogeneic transplant can be done on an outpatient basis. This means you do not have to stay in the hospital or medical center.
How long you stay in the hospital depends on how much chemotherapy or radiation you received, the type of transplant, and your medical center's procedures. While you are in the hospital, you will be isolated because of the increased risk of infection. The health care team will closely monitor your blood count and vital signs.
While you are in the hospital you may:
• Receive medications to prevent or treat infections, including antibiotics, antifungals, and antiviral drugs.
• Need many blood transfusions
• Be fed through a vein (IV) until you can eat by mouth and stomach side effects and mouth sores have gone away
• Be given medication to prevent graft-versus-host disease
Recovery
The new bone marrow normally takes almost a year in order to function normally. During this period the patient is to be monitored closely to identify any infections or complications that may develop. The recovery process continues for several months or longer after discharging from the hospital, during which time the patient cannot return to work or many previously enjoyed activities.
You may want to ask some questions before your treatment begins:

Mr.Gilbert, Knee Replacement, Nigeria
Mr.Gilbert from Aba, Nigeria who came to India for his knee replacement in India.
Mrs. Kalangwa George, Lung Cancer, Kenya
Mrs. Kalangwa George from Mombasa, Kenya who came to India for her Lung Cancer Treatment in India.
Mrs. Elisabeth, Breast Cancer Surgery, Nigeria
Mrs. Elisabeth from Kano, Nigeria who came to India for the Breast Cancer Surgery.
Mr.Tselmeg, Kazakhstan, Spine Surgery
Mr.Tselmeg from Astana, Kazakhstan who came to India for the Spine Surgery
Mr. Stephen Okafor, Spine Surgery, Nigeria
Mr. Stephen Okafor from Onitsha, Nigeria who came to India for the Spine Surgery
Mrs. Asiata Nofiu, Laparoscopic Ovarian Cystectomy , Nigeria
Mrs. Asiata Nofiu from Lagos, Nigeria who came to India for the Laparoscopic Ovarian Cystectomy
Mr. Alhassan Osman, Prostate Treatment, Tanzania
Mr. Alhassan Osman from Mwanza, Tanzania who came to India for the Prostate Treatment
Mr. Okubowa Babatunde , Heart Surgery , Zimbabwe
Mr. Okubowa Babatunde from Harare, Zimbabwe who came to India for the heart hole surgery